There are many techniques in physical therapy to help reduce muscle spasms. Muscle spasms (or “trigger points”) are those nasty kinds of pains that we often get in our necks and backs as a consequence of carrying a lot of tension in our lives or from overworking at the computer. Also, these spasms sometimes come on in response to injuries (as a “guarding” mechanism) even after the primary injury has been remedied. For many years, I, as a physical therapist, have treated these muscle pains with massage, exercise, ultrasound, electrical stimulation with good results, but I’ve always wanted to find a way to increase my effectiveness. Since 2012, the North Carolina Physical Therapy Practice Act has included dry needling as part of what physical therapists can include in their rehabilitation, and this has made a considerable positive difference in my practice as a physical therapist.
So, you might be asking the question, “What is dry needling, anyway?” Well, dry needling is a procedure done by health care practitioners where a filiform needle (small solid needle of 0.3 millimeters diameter) is inserted into the muscle where it is sore, with the intention of causing a twitch response which then allows the muscle to relax. When the muscle relaxes, the pain diminishes or goes away.
Wherever there are muscles in the body that have sensitive or active trigger points contributing to a painful problem, dry needling can be used to help. For example, individuals with neck pain and headaches often come into the clinic seeking relief.
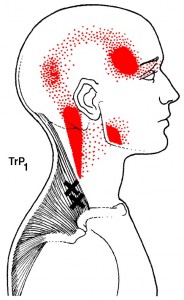 Please note the XX’s in the diagram to the left, as they show trigger points. The trigger points then “refer” (send painful sensations) to the areas shown in the red. So it is easy to see how when trigger points are active, they can send patterns out to the head, causing headache symptoms.
Please note the XX’s in the diagram to the left, as they show trigger points. The trigger points then “refer” (send painful sensations) to the areas shown in the red. So it is easy to see how when trigger points are active, they can send patterns out to the head, causing headache symptoms.
There was an individual who came into the clinic recently who had just this distribution of trigger points – they reported pain in the neck and headaches. Physical therapy was started, and dry needling was instrumental in helping to reduce the sensitivity of the trigger points, thereby improving the neck pain and headaches.
In another example of how dry needling made a difference in patient outcomes, there was a woman who was a runner who came into the clinic complaining of runner’s knee pain.
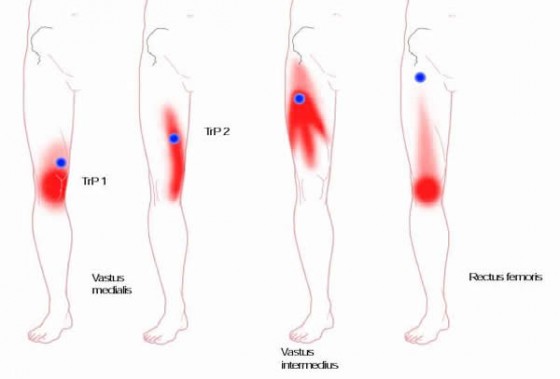
As you can see from the diagrams below, the sensitive areas refer pain right around the knee area where runners have knee pain. By all means, there are more reasons than trigger points that cause knee pain (e.g. poor mechanical posture of the knees, ligament or cartilage sprains, or tears and weakness around the knee), but these trigger points can be a significant part of helping people with knee pain more successfully and efficiently work through the problem.
It is important to note that dry needling by itself is not the best way to correct a trigger point or muscle spasm concern. A trigger point problem needs to be understood as a stress reaction to the muscle, and the reason for that stress should be found out and corrected so that trigger point does not re-surface as a problem again in the future. Understanding and comprehensively managing the problem is the key to physical therapy resolution of musculokeletal problems!

